CPAP vs BiPAP – What are the differences and which one do you need?
Sleep apnea is a common sleep disorder in which breathing repeatedly starts and stops. Those with sleep apnea typically feel tired even after a full night’s sleep, followed by morning headaches and irritability.
Sleep apnea affects 3% to 7% of the population, making it one of the most common sleeping disorders out there. While this condition can be a nuisance to the lives of those who have it, there are treatment options that help. Although there are CPAP pillows and other types of sleep medicine, the most common treatment options for sleep apnea include CPAP and BiPAP therapy.
Continuous positive airway pressure (CPAP) is the most common PAP treatment, but bi-level positive airway pressure (BiPAP) works better for others. While they both work in similar ways, there are key differences between the two that determine their effectiveness for your specific condition. So, what is are the differences between CPAP vs BiPAP, and what do they treat?
What Is the Difference Between CPAP and BiPAP Machines?
CPAP and BiPAP machines work in similar ways, but work to treat different types of sleep apnea. There are three types of sleep apnea including obstructive sleep apnea, central sleep apnea, and mixed sleep apnea. Because each of these forms like obstructive sleep apnea and central sleep apnea can have potential impacts on one’s health, it’s important to know the difference between BiPAP vs CPAP machines so you know the best option for your needs.
Differences in CPAP machines and BiPAP machines can be defined as the number of pressure settings each one provides.
– With a continuous positive airway pressure machine (CPAP), patients receive a single pressure of continuous airflow through the face mask.
On the other hand, a BiPAP machine provides two pressure settings:
– one for inhalation and a lower pressure for exhalation. Because of this, many patients with sleep apnea find the BiPAP more comfortable as it’s more customizable for a patient’s needs.
In CPAP and BiPAP machines, pressurized air from the machine is forced down the airway in order to keep it open and free from obstruction, allowing patients to breathe consistently throughout the night. When CPAP therapy cannot be tolerated, that’s when BiPAP therapy comes into play with the two pressure options it provides.
For both CPAP and BiPAP machines, it’s important to keep your mask and tubing clean throughout its use. This can be done using a CPAP cleaner or soap that’s meant to clean the mask.
In order to make the switch from a CPAP machine to a BiPAP machine, patients must seek medical advice from a doctor so they can approve the switch between these pressure machines in order to be covered by insurance.
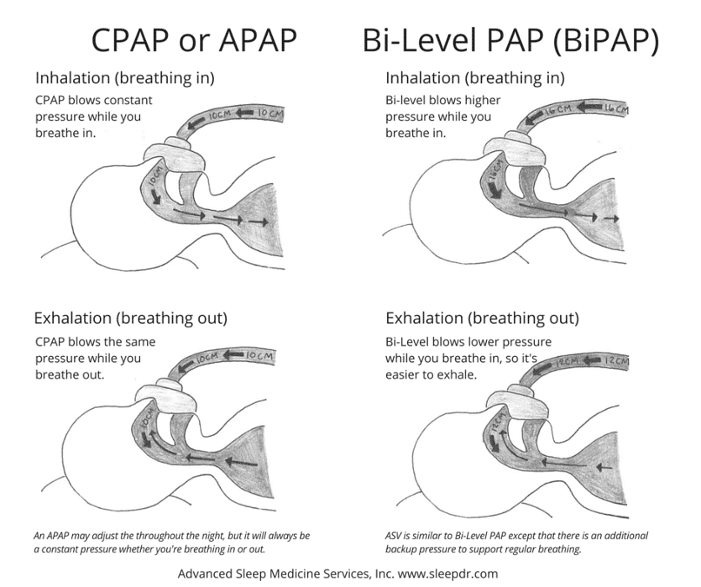
CPAP Explained

A continuous positive airway pressure machine provides a single pressure of continuous airflow through a full face mask that’s worn while patients sleep to aid their breathing. This pressure that the machine provides is said to both prevent pauses in breathing and snoring, as well used to treat other symptoms that come with having the condition, including:
- Excessive daytime sleepiness
- Insomnia
- Nightmares
- Dry mouth
- Headaches
- Irritability
CPAP machines feature an adjustable pressure setting that ranges from 4 to 20 cm H2O while the user is breathing. Typical medical applications for CPAP machines are used to treat obstructive sleep apnea (OSA) and the use of the machine for preterm infants.
Obstructive sleep apnea has a major impact on cardiovascular function and has been associated with conditions such as congestive heart failure and hypertension. This condition can also overlap with chronic obstructive pulmonary disease (COPD), which can cause long-term chronic health problems.
In order to determine the proper amount of airflow pressure that you need to treat your sleep apnea, talk to your physician so they can evaluate based on your needs. This is typically determined based on your anatomy or weight, or through a sleep study for a more in-depth look at your condition.
Those with sleep apnea typically start treatment with CPAP machines. This condition is often brought up by those who have had heart failure, a stroke, or those who use narcotic pain medications.
BiPAP Explained

Bi-level positive airway pressure therapy (BiPAP) features two air pressure settings that the device is able to alternate between while the patient is breathing at night. With each pressure setting, patients can switch between the higher and lower pressures and inhale with higher pressure and exhale with slightly lower pressure with the full face mask on at night. Most BiPAP machines feature a range of 4 to 25 cm H2O, which is 5 cm higher than CPAP machines.
The two air pressure settings featured in a BiPAP machine include one higher pressure for inhalation called IPAP, and one lower pressure for exhalation, called EPAP. The BiPAP machine itself has up to three settings for the switch between IPAP and EPAP:
The first air pressure setting in a BiPAP machine is a timed switching setting, allowing the user to adjust how long the IPAP and EPAP pressures last. This customizable feature ensures users are able to take the correct number of breaths per minute, so they get the proper treatment for their condition.
Second, the machine has spontaneous switching options that sense the user’s breathing pattern and switch between the IPAP and EPAP air pressure settings. This setting is standard for BiPAP machines, as most users rely on the setting for a restful sleep at night.
Lastly, spontaneous/timed switching combines the first two settings, as timed switching turns on when the device detects that the user’s breathing has dropped below a set number of breaths per minute. This intricate setting also follows the user’s natural breathing patterns.
BiPAP vs CPAP: Which is Best for You?
In order to make the best choice for your condition, we must compare BiPAP vs CPAP therapy to know the difference between the two. Continuous positive airway pressure therapy (CPAP) uses a machine to treat obstructive sleep apnea (OSA) which helps keep the patient’s airway open and helps them breathe better during their sleep at night. Obstructive sleep apnea is the most common form of this condition.
As for BiPAP machines, these devices are often used to treat central sleep apnea (CSA) and complex sleep apnea as well as heart, lung, and neurological disorders that require structured airway support while patients sleep. Treating complex sleep apnea forms with sleep medicine and a BiPAP machine or CPAP machine is crucial in preventing long-term effects on your health.
For the most part, those with sleeping disorders like sleep apnea start off with a CPAP machine for their therapy treatment. When patients first use a CPAP machine with the CPAP mask, there’s typically an adjustment period before you’ll feel comfortable using the device.
If you experience discomfort with CPAP therapy, it can be managed by adjusting the pressure settings, trying different mask types, and experimenting with climate control accessories for those that feature the option.
If you try the continuous positive airway pressure machine for your sleep apnea and you feel the CPAP therapy isn’t right for you, it’s important that you consult a doctor about the possible switch from CPAP to BiPAP therapy. This switch between these pressure machines must be decided on by a doctor and supervised by a sleep specialist in order to verify that the transition is right for your treatment.
If you suspect that you have sleep apnea, contact your primary care doctor. Your doctor may refer you to a sleep specialist to further assess your condition and possibly conduct a sleep study. The machine will then need to be approved by the sleep specialist or doctor for it to be covered by insurance. If left untreated, sleep apnea can increase the risk of serious health problems, making it important that the condition is dealt with as soon as possible.
CPAP vs BiPAP Takeaways (Key Features & Differences):
CPAP
- Continuous Pressure
- Same pressure during exhalation and inhalation
- Used at home
- Usually a simple device
- Needs little monitoring
- Cheaper than BiPAP
BiPAP
- Continuous Pressure
- Pressures are different between inhalation and exhalation (5cmH2O exhalation vs 15cmH2O inhalation)
- Not commonly used at home
- No simple devices
- Pressures need monitoring
- Expensive


